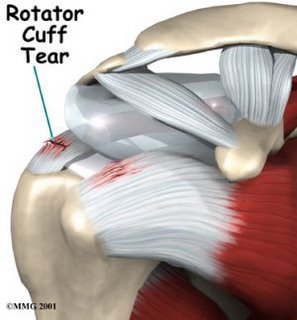
 Sometimes surgery for rotator cuff problems are unavoidable, especially if you have an actual tear.
Sometimes surgery for rotator cuff problems are unavoidable, especially if you have an actual tear.What are the implications for those either at risk for or already have lymphedema?
Clinical studies indicate good sucess with this surgery. There appear to be the normal swelling post-op and even in lymphedema patients it usually subsides. See the initial article for a study done on this.
There are no studies on the at risk patient that I am aware of. From my own personal experience, an individual I know who is highly at risk for lymphedema (several family members have it) has experienced off and on swelling. It may be too early to accurately know what will happen.
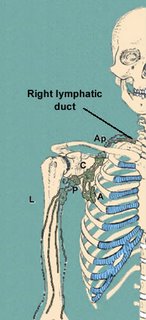
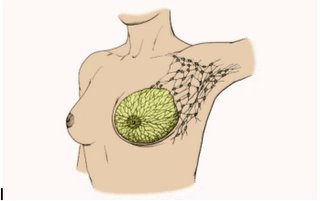
In either event, it is imperative that the surgeon understand the possibilities of lymphedema and understand the location of the lymph nodes in this area. Picture below give illustrations.
Lymphedema Preoperative Considerations:
1. For the prevention of infection and/or to lower the risk of infection it may be necessary for you to be on a preventative therapy of antibiotics BEFORE surgery.
2. For the prevention of blood clots (venous thrombosis) and based on any additional underlying medical conditions, you should also discuss the possibility of being on blood thinners before the surgery.
3. Make arrangements and plans for the scheduling and/or resumption of decongestive massage therapy for the lymphedema after the surgery.
4. Be sure to have your PCP, surgeon and lymphedema therapist working together to design a treatment/therapy modality that is best for you.
5. Familiarize yourself with the rotator cuff surgery so that you will know what to expect.
6. With consideration of surgical complications, it is important to try all methods of treatment before a surgery is planned.
7. What are the considerations of the need for a future second surgery affect your lymphedema.
8. If you are obese or morbidly obese discuss how the added strain of the surgery will affect your lymphedema.
9. Be sure to understand the specifics of what you can or can't do, how long you will be off work, financial arrangement and the need for personal assistance you may have.
Possible Complications
Complications include possible infections, especially around an the incision, damage to nerves or blood vessels and of special concern to those with lymphedema, the lymph nodes of the region.
General Patient Post-Operative Considerations Here are some do’s and don’ts for when you return home:
Do wear the sling every night for at least the first month.
Don’t use your arm to push yourself up in bed or from a chair because this requires forceful contraction of muscles.
Do follow the program of home exercises prescribed for you. You may need to do the exercises 4 to 5 times a day for a month or more.
Don’t overdo it! If your shoulder pain was severe before the surgery, the experience of pain-free motion may lull you into thinking that you can do more than is prescribed. Early overuse of the shoulder may result in severe limitations in motion.
Don’t lift anything heavier than a cup of coffee for the first 6 weeks after surgery. Do ask for assistance. Your physician may be able to recommend an agency or facility if you do not have home support.
Don’t participate in contact sports or do any heavy lifting for at least 6 months.
Contact your Physician if
Pain, swelling, soreness or redness in the arm Increase in shoulder pain Fever Discharge, pus or smelly drainage Sudden or unexplained re-swelling of joint (after initial post operative swelling has decreased) If the arm was not swollen before surgery, immediate report any post-operative edema.
These illustrations show which lymph nodes are in the general area and may be effected
The Surgery
Rotator cuff surgery is a highly technical procedure; each step plays a critical role in the outcome.
After the anesthetic has been administered and the shoulder has been prepared, a cosmetic incision is made over the top front corner of the shoulder.
This incision allows access to the seam between the front and middle parts of the deltoid muscle. Splitting this seam allows access to the rotator cuff without detaching or damaging the important deltoid muscle, which is responsible for a significant portion of the shoulder's power. All scar tissue is removed from the space beneath the deltoid and the acromion (part of the shoulder blade to which the deltoid attaches). Thickened bursa and the rough edges of the rotator cuff and humerus (upper arm bone) are also smoothed to make sure that they pass smoothly beneath the acromion and deltoid.
The edges of the cuff tendons are identified and the quality and quantity of the cuff tissue is determined.
The goal of the repair is to reattach good quality tendon to the location on the arm bone from which it was torn. If the tendon cannot reach this spot with the arm at the side of the body, the shoulder surgeon releases the tendon from the surrounding tissues. If good quality tendon will not reach its attachment site after these releases, the cuff tear is deemed to be irreparable. In this situation the useless tendon is cut out and the shoulder is again examined to assure smooth and full motion. Again, achieving this smooth movement may require trimming of the tendon edges or the bone of the upper humerus. Occasionally, it may be necessary to perform an acromioplasty, a procedure in which part of the bone overlying the rotator cuff is removed. Acromioplasty is avoided unless it is necessary because it increases the risk of weakening the deltoid and causing scar tissue.
If the rotator cuff is repairable, a groove or trough is fashioned in the normal attachment site for the cuff.
Sutures (lengths of surgical thread) draw the edge of the tendon securely into the groove to which it is to heal. This method of attachment leaves a smooth upper edge of the cuff repair to glide beneath the acromion and deltoid and avoids possible problems with suture anchors. After the cuff is repaired, the deltoid muscle and skin are closed.
Because the deltoid is not detached from the acromion in this surgical approach, it is called the "deltoid on" approach.
Anesthetic Rotator cuff surgery may be performed under a general anesthetic or a brachial plexus nerve block. A brachial plexus block can provide anesthesia for several hours after the surgery. The patient may wish to discuss their preferences with the anesthesiologist before surgery.
Length of rotator cuff surgeryRotator cuff surgery usually takes approximately one hour. However, the preoperative preparation and the postoperative recovery may add several hours to this time. Patients often spend two hours in the recovery room and about two days in the hospital after surgery.
Recovery of comfort and function after cuff surgery continues for a year after surgery.
Rotator cuff surgery is a major surgical procedure that involves cutting of skin, release of scar tissue, and suturing of tendons and bone. The pain from this surgery is managed by the anesthetic and by pain medications. Immediately after surgery, strong medications (such as morphine or Demerol) are often given by injection. Within a day or so, oral pain medications (such as hydrocodone or Tylenol with codeine) are usually sufficient.
Initially, pain medication is administered usually intravenously or intramuscularly. Sometimes patient controlled analgesia (PCA) is used to allow the patient to administer the medication as needed. Hydrocodone or Tylenol with codeine are taken by mouth. Intravenous pain medications are usually needed only for the first day or two after the procedure. Oral pain medications are usually needed only for the first two weeks after the procedure.
Pain medications can be very powerful and effective. Their proper use lies in the balancing of their pain relieving effect and their other, less desirable effects. Good pain control is an important part of the postoperative management.
Pain medications can cause drowsiness, slowness of breathing, difficulties in emptying the bladder and bowel, nausea, vomiting, and allergic reactions. Patients who have taken substantial narcotic medications in the recent past may find that usual doses of pain medication are less effective. For some patients, balancing the benefit and the side effects of pain medication is challenging. Patients should notify their surgeon if they have had previous difficulties with pain medication or pain control.
After surgery the patient spends an hour or so in the recovery room. A drainage tube is sometimes used to remove excess fluid from the surgical area. The drain is usually removed on the second day after surgery. Bandages cover the incision. They are usually changed the second day after surgery.
Recovery and rehabilitation in the hospital
Shoulder motion soon after rotator cuff surgery helps achieve best possible shoulder function. Shoulders with cuff disease may have substantial scarring and may be stiff. One of the major goals of rotator cuff surgery is to relieve any stiffness. However, after surgery scar tissue will tend to recur and limit movement unless motion is started immediately. This early motion is facilitated by the complete surgical removal of the scar tissues so that after surgery the patient needs only to maintain the range of motion achieved at the operation.
A continuous passive motion (CPM) machine is often used to gently move the shoulder in the recovery room immediately after surgery. The CPM, shown in figure 6 and movie 1, is continued for the first few days after surgery whenever the patient is in bed.
During the hospitalization, the patient learns a simple rehabilitation program that will be used to maintain the range of motion at home after discharge.
Figure 7 shows the exercises used to maintain elevation and rotation of the arm. On the day of surgery or on the day after, the physical therapist teaches the patient gentle range of motion exercises. Usually, the patient is shown how to stretch the shoulder forward and out to the side, preventing stiffness and adhesions.
QuickTime movie
Movie 1: Continuous passive motion machine (1.70 MB)
Patients are discharged as soon as:
the incision is dry,
the shoulder is comfortable with oral pain medications,
the patient feels comfortable with the plans for managing the shoulder,
the patient can perform the range of motion exercises, and
the home support systems for the patient are in place.
Discharge is usually on the second or third day after surgery.
Walking and use of the arm (with the elbow at the side) for gentle activities are encouraged soon after surgery.
If a cuff repair has been performed, the arm must be used only with the elbow at the side and only for very gentle activities so that the repair is protected. These precautions remain in place for three months until the initial healing of the cuff repair is complete.
The patient's specific limitations can be specified only by the surgeon who performed the procedure. It is important that the repaired tendons not be challenged until they have had a chance to heal. Usually the patient is asked to lift nothing heavier than a cup of coffee (with the elbow at the side) for the first three months after the surgery.
Management of these limitations requires advance planning to accomplish the activities of daily living during the period of recovery.
Patients usually require some assistance with self-care, activities of daily living, shopping, and driving for approximately three months after surgery. Patients usually go home after this surgery, especially if there are people at home who can provide the necessary assistance, or if such help can be arranged through an agency. In the absence of home support, a convalescent facility may provide a safe environment for recovery.
Recovery of comfort and function after rotator cuff surgery continues for many months after the surgery. Improvement in some activities may be evident as early as three months. With persistent effort, patients make progress for as long as a year after surgery.
Effects of general health on healing
The healing after rotator cuff surgery can be compromised by smoking, poor nutrition, and medications such as cortisone. Diabetes can cause additional scar tissue. Heart and lung disease, as long as they are well managed, do not seem to have an effect.
See entire excellent section on the surgery:
For additional Information:

11 comments:
This blog contain a great information about Lymphedema.By reading this useful blog basically I know about Lymphedema and its prevention also.This information gives a more conscious about this disease.Thanks for creating this type of informative blog.
I have been looking for answers as to why I have lymphedema in my neck and clavicle area in both sides. Maybe it did start with the rotator cuff/labrum/bone spur surgery I had. I didn't notice it until a year after the surgery, but maybe that is when it got bad. My doctors haven't seemed to care why I have lymphedema.
I was told the surgery was a blood bath, so maybe the surgeon couldn't see to do whatever about lymph glands. I know of a great aunt that had severe lymphedema, no one else so I wouldn't know to be concerned about this.
I don't know what to do now, my massage therapist helps, but I just don't know.
I have had both shoulders affected with torn rotator cuffs, torn lab rums, bone spurs and severe arthritis, except only one side was operated on (long story). It has been 2-3 years since the surgery. I started getting big swelling around both clavicles and neck area for over a year. No known cancer, that has concerned me that something was possibly there and not found.
I have never thought of it possibly being caused by the shoulder surgery. I hope that is the case and not tumors. Yes, I have had over 3 doctors recognize that I get lymphedema in that area. My massage therapist does some lumph massage.
I don't know if anyone else is like this, but one side will suddenly swell like a baseball and I have horrible aching all over etc.
Hi Lynda, I would garner to say it is lymphedema too as a result of the surgery. My older sister had the exact same thing happen after a rotator cuff surgery on her right arm.
There are some garments that might help, ask your therapist about them. If they don't know, drop another note and I will see what I can do. Pat
What a great blog. Its inspirational and mouthwatering all at the same time.
Pelvic Pain Treatment
Shoulder surgery is repairing the tissues within and around the shoulder joint. It is one of the most delicate yet complex joint of human body which is vulnerable to outer stress and injuries.
I had surgery Feb. 26, 2018. My bi-cept was frayed, they did some shaving and cleanup. I have still got swelling in my arm and neck and left side of chest/breast. They did an ultra sound to eliminate the possibility of blood clots. I have RA and am on Methatrexate which frightens me due to Lymphoma being a potential side effect! If Lympedema is the cause, I need all the advise I can get!
Nice Post. It’s really a very good article. I noticed all your important points. Thanks
Hair Restoration
Hip Replacement Surgery
Shoulder Surgery
PRP Hair Treatment
Shoulder Treatment
prp knee treatment
PRP Hair Treatment
Shoulder Surgery
Elbow Surgery
alternatives to knee surgery
alternatives to hip surgery
alternatives to shoulder surgery
alternatives to elbow surgery
Knee Injury and Arthritis Stem Cell Treatment
Shoulder Injuries and Arthritis Stem Cell Therapy
Bio Facial Skin Rejuvenation
I was diagnosed of Herpes 2 years ago and I have tried all possible means to get the cure but all to no avail, until I saw a post in a health forum about a Herbal Doctor(Dr Akhigbe) who prepares herbal medicine to cure all kind of diseases including Herpes, at first i doubted, if it was real but decided to give him a trial, when I contacted Dr Akhigbe through his Email: drrealakhigbe@gmail.com he guided me and prepared a herbal medicine and sent it to me via courier Delivery service,when I received the package (herbal medicine) He gave me instructions on how to consume it,I started using it as instructed and I stopped getting outbreaks and the sores started vanishing, could you believe I was cured of this deadly virus within two to three weeks and notices changes in my body. Days of using this REMEDY,couldn't believe the healing at first until I see it as my HERPES get cleared like magic Dr Akhigbe also use his herbal medicine to cure diseases like, HIV, HERPES, CANCER, ALS, CHRONIC DISEASE, HEART DISEASE, LUPUS, ASTHMA, DIABETES HEPATITIS A AND B.ECZEMA, BACK PAIN, EXTERNAL INFECTION ,ASTHMA, MALARIA, DENGUE FEVER, BACTERIA DIARRHEA, RABIES, OBESITY, PROGERIA, MENINGITIS, EPILEPSY,STROKE, LYMPHEDEMA, GALLSTONE, PENIS EJACULATION, HPV, OSTEOPOROSIS, RHEUMATISM, THYROID, COLD & FLU,KIDNEY DISEASE,ACME. ERYSIPELAS. etc Contact this great herbal Doctor today the father of herbal root cure. via Email: drrealakhigbe@gmail.com or whatsapp him +2349010754824 and get cured permanently He is real..website: https:drrealakhigbe.weebly.com
I have been suffering from a deadly disease (Hsv) for the past 2 years now, I had spent a lot of money going from one places to another, from churches to churches, hospitals have been my home every day residence. Constant checks up have been my hobby not until this faithful day, I was searching through the internet, I saw a testimony on how Dr Ehimare helped someone in curing his (Hsv) herpes disease, quickly I copied his email which is drehimare3@gmail.com just to give him a test I spoke to him, he asked me to do some certain things which I did, he told me that he is going to provide the herbal cure to me, which he did, then he asked me to go for medical checkup after some days after using the herbal cure, behold I was free from the deadly disease, he only asked me to post the testimony through the whole world, faithfully am doing it now, please brothers and sisters, he is great, I owe him in return. if you are having a similar problem just email him on Drehimare3@gmail.com Or whatsapp him via +1 (267) 691-1087
Post a Comment